
Today we start doing what we came here to do, saving smiles and changing lives. The surgical team, under the careful direction of Debby Dean, RN has their schedules, instructions, and everything in place and ready for the first patients.
The schedule is different for this mission, as there are fewer cleft palates and lips and more burn injuries that need work. In order to sort through the nearly one hundred potential patients, priorities were set that were sometimes hard for some parents and patients to understand. I have the unique position as the photojournalist to move freely among the patients, staff, and mission people and listen to the stories and in some cases, questions. I was asked numerous times why some procedures were done and others not. With the cleft palates and lips, the priority is to make the most impact on the patient’s life as possible. This means getting the right surgeries done as early as possible to enhance their physical and speech development and overall quality of life. In some cases this means doing a lip one year and the palate on the next mission. The top priority goes to those problems with children age six and younger.
The second priority goes to cleft palates and lips for children over 6 years old and burn restoration that restores functionality. It’s difficult to explain to a parent, especially one who has traveled far and has high expectations that, even with the best of surgeons, their child isn’t going to be perfect cosmetically. Sometimes, especially with burns, there is only so much that can be done so the priority goes to releasing contractures. In many cases, as burns heal, the motion becomes restricted by scar tissue and the range of motion is radically reduced or stopped altogether. The skin may heal looking like a web between the fingers or connecting the upper and lower arms for example. The goal is to release the contracture, restore as much range of motion as possible, and improve the quality of life.
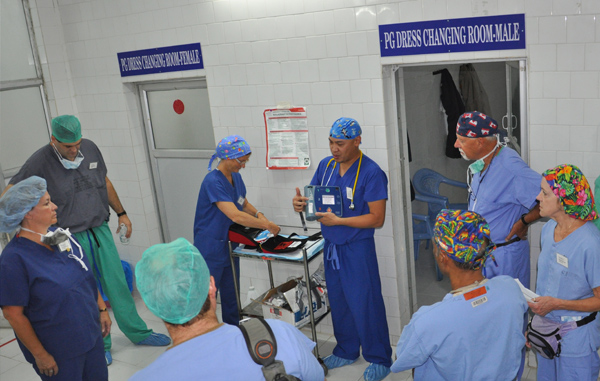
Safety First! The team rehearses what to do in case of emergency, where each piece of life saving equipment is and who is responsible for what. Working in a strange operating room a half a world away from home is difficult enough but when language differences are taken into account, things can really get confusing.
Patients first meet Amie Shaw, DO, Pediatrician in the pre-op ward which is down the hall way leading to the surgical suite. Dr. Shaw confirms that pre-operation instructions have been followed and that the correct patients are ready for surgery. More than once patients have not shown-up, or come on the wrong day, or in one case, tried to sign in as someone else. Pre-op can be noisy with patients pushing forward to find out when their turn is.
Once cleared by Dr. Shaw, patients are transport to the surgery suite by Alan Shirley and Joe Renaldo where they’re handed over to the anesthesiologists who get the patients to “ take a little nap” and get them asleep and ready for the surgeons.
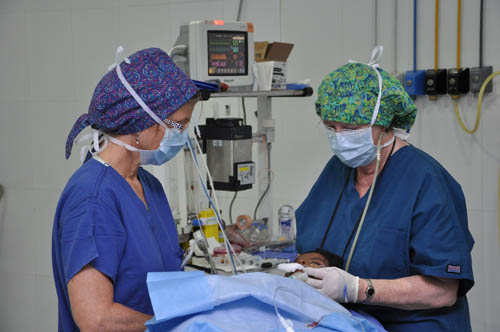
Anesthesiologist Helen O'Keffe Vajk, MD and OR Nurse Gina Brown, RN get a patient ready for surgery.
It still amazes me the smooth confidence with which the surgeons work. I watch them evaluating, planning, and once the plan is firmly in mind, implementing the plan. Whether it is a simple lip procedure or a more complicated burn restoration, surgery just flows. They work with local national nurses and residents in the operating rooms, teaching as they work.
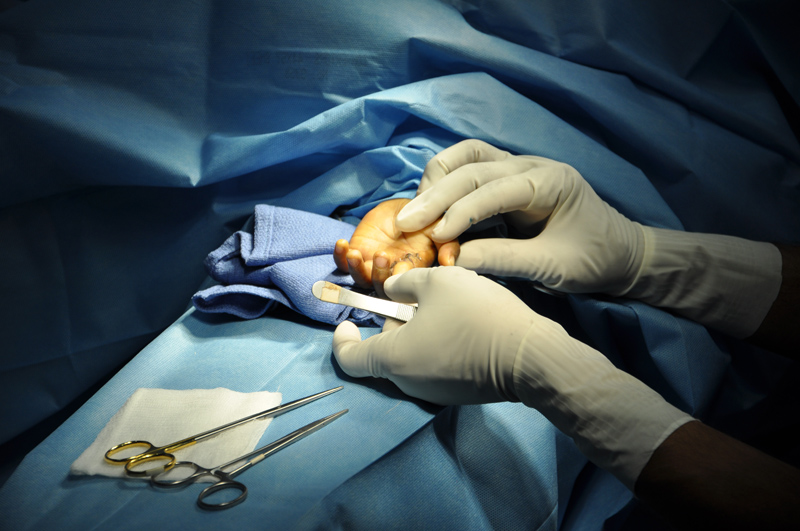
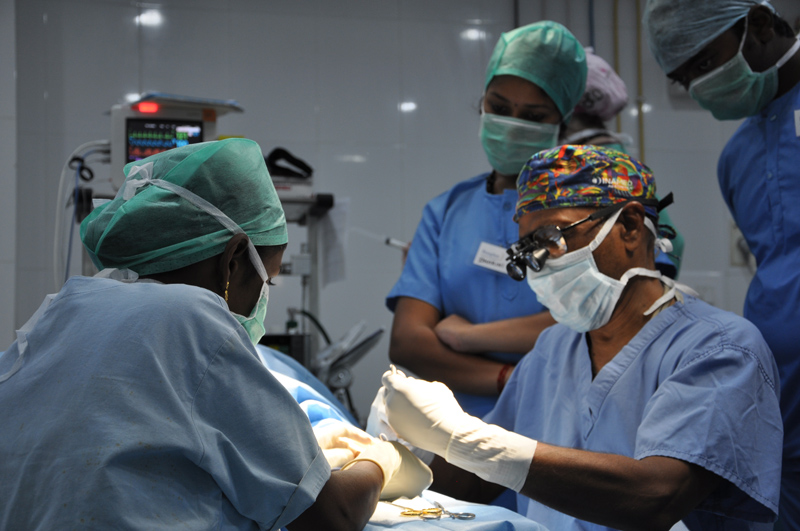
Dr. Soma works on a tiny hand, releasing a contracture and restoring function.
Part of the joy of this volunteer work comes in the moment the team reunites a parent with their child after surgery. The patients move from surgery to the PACU, the post anesthesia care unit, to recover from the effects of anesthesia. Under the watchful eye and constant care of Lead PACU Nurse Bruce Hickey, RN, and Wendell Alderson, RN PACU Nurse, patients gradually recover from the effects of anesthesia. Once the PACU nurses determine that all is well and the patient is stable, staff brings a parent in to be with the child as they wake up.
It’s easy to see the relief as they realize the child is ok and then the wonder of seeing the new lip. I often smile as I watch a baby, not quite awake, exploring her new lip with her tongue, discovering a new sensation. It’s at this moment in time that all the effort, endless hours of travel, working in less than ideal conditions, and suffering the heat, culminates in a life that has been changed. An impact has been made on this family and the future has been forever changed and improved.




