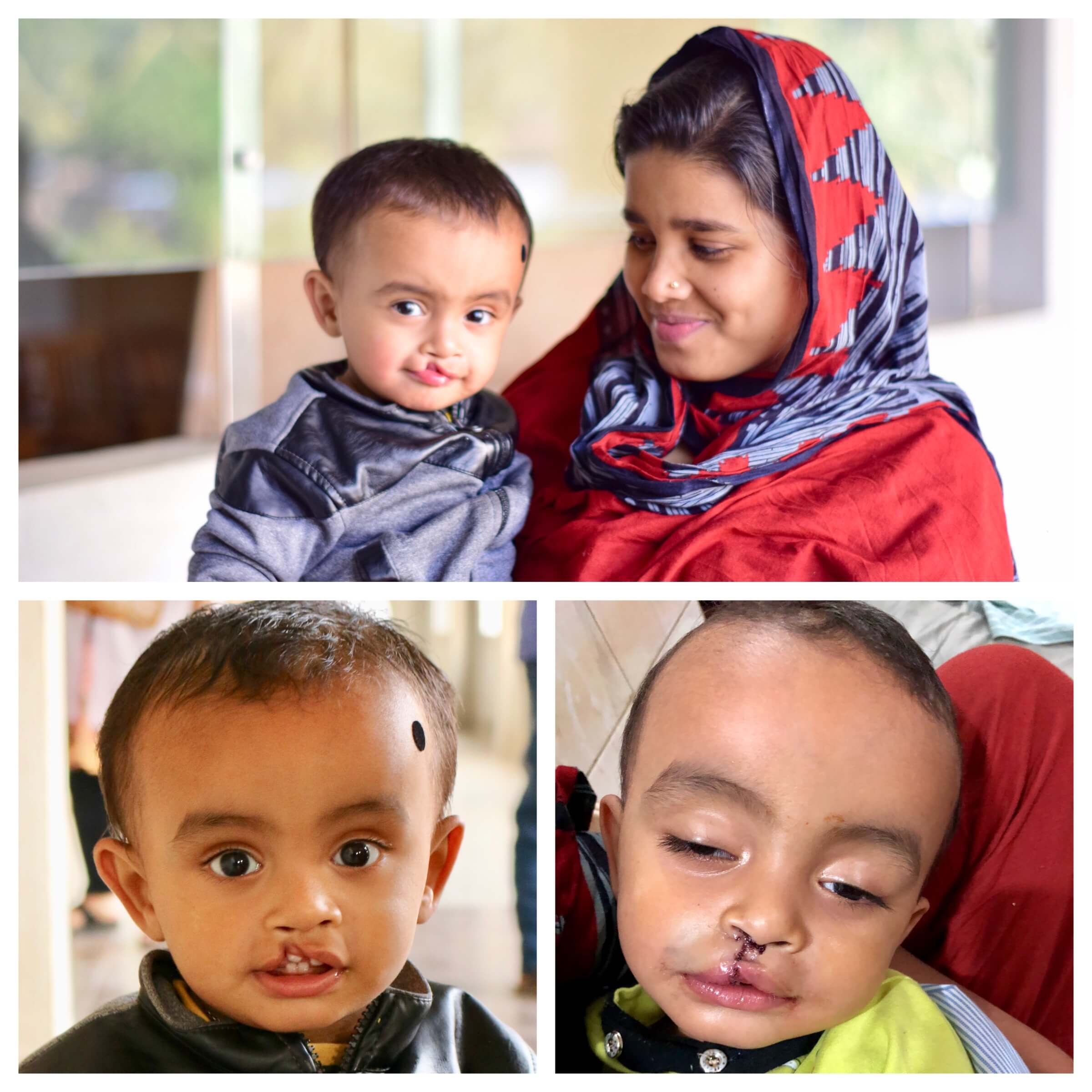
Operation days are the most exciting days for me. I wake up hours early, envisioning in my mind the arm strokes of the Surgeons as they craft a new face. Or the look on a parent’s face when they see their child for the first time post-op. But most people are not filled with so much joy the morning of an operation. A large reason people are afraid of surgery is that it carries so much “unknown” for the common person. It is one of the most vulnerable positions to be in— asleep in a room of strangers who will be performing a medical procedure on what is most likely an injured area of the body. What will the outcome be? What is going to happen? In today’s blog, let’s demystify the latter and walk step by step for what happens during a typical Rotaplast operation.
First, medical staff arrive at the hospital, call next day patients for reminder, change clothes for a sterile environment, and begin preparing their room and testing the equipment they will need.

[Pictured L->R, T->B: Marilyn Santiago (OR Nurse), Wally Chang (Surgeon), local Roteract member, Tony Scheppmann (Medical Records), David Stellway (Anesthesiologist), Mohammed Hannan (CRNA), Michael Fallon (Anesthesiologist), Katherine Gallagher (Lead Pediatrician)]
Patients anxiously wait in the Wards so we can monitor them pre-surgery, especially to ensure they haven’t had anything to eat or drink which could put them at risk during the surgery. A Recreation Therapist brings games or toys to occupy the patients as they wait. The Pediatrician/Pediatric Nurse Practitioner goes bed to bed to confirm no one has become ill and that they are still well enough for their operation. The surgeon will also come and re-inspect the area of interest to confirm their operation plan.

[Pictured: Monica Morales (Ward Coordinator) and Diana Deleon (Recreation Therapist) with patients]
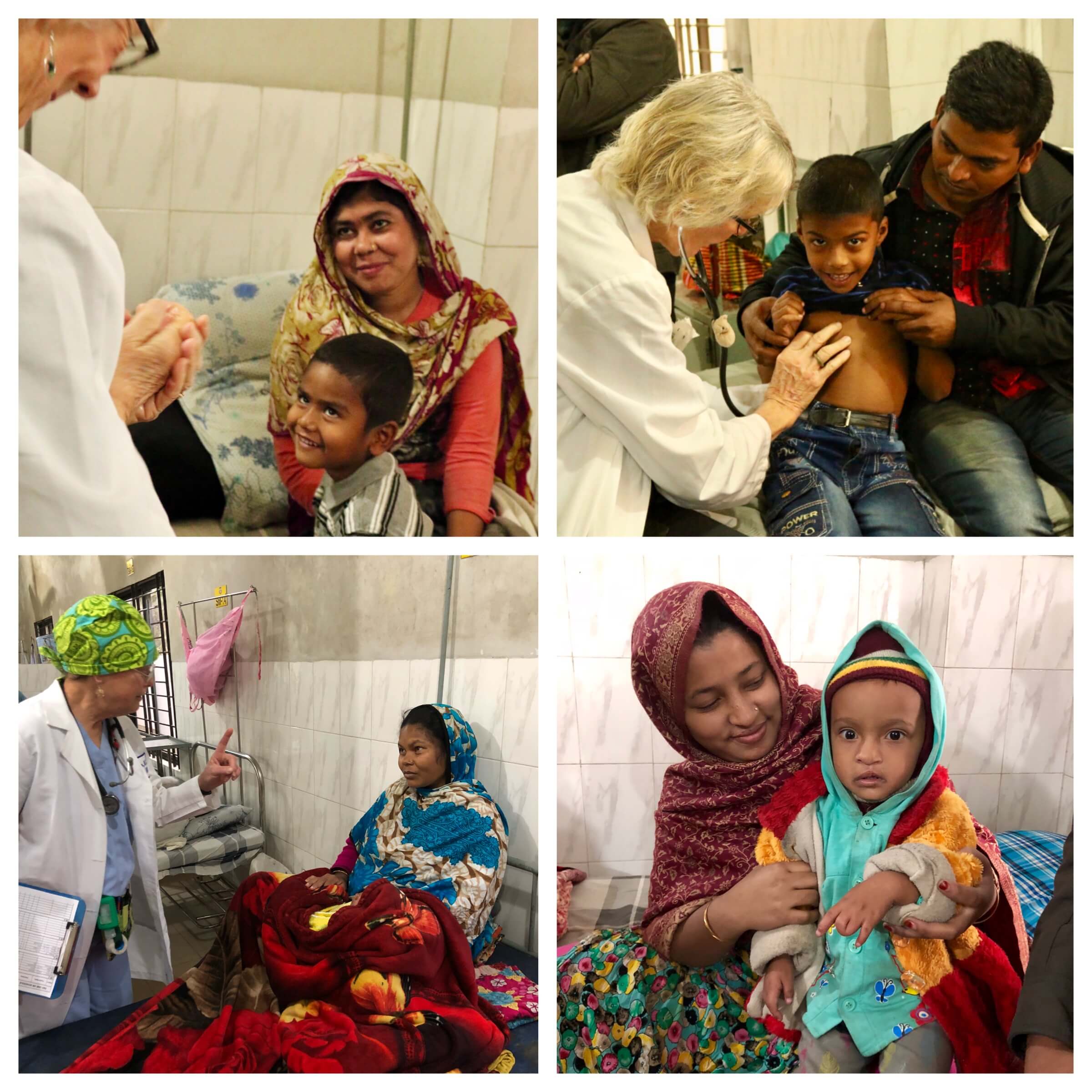
[Picture: Nan Madden (PNP) and Katherine Gallagher with patients]

[Pictured: Milton Solis (Surgeon) with patient]
When it is their turn, the patient and family will be taken to a waiting room and ultimately carried or walked into the operating theater. Usually an adult patient will already have an IV of salt water ready to go, whereas a child will get their IV only after they are asleep to minimize discomfort.

[Pictured: Marilyn Santiago carrying patient, Randy Floyd (Mission Director), Monica Morales bringing patient back to OR]
Upon entrance into the operating room, a patient will be hooked up to several diagnostic machines to monitor the brain, blood pressure, heart rate, and oxygen saturation which will be used to analyze how well the patient is withstanding the surgery. Then they will be given a mask flowing Oxygen and then ultimately an Anesthetic that puts them to sleep. The team will perform a “time out” where they review the case one more time before beginning which will include confirming patient and location of injury, among other descriptions.
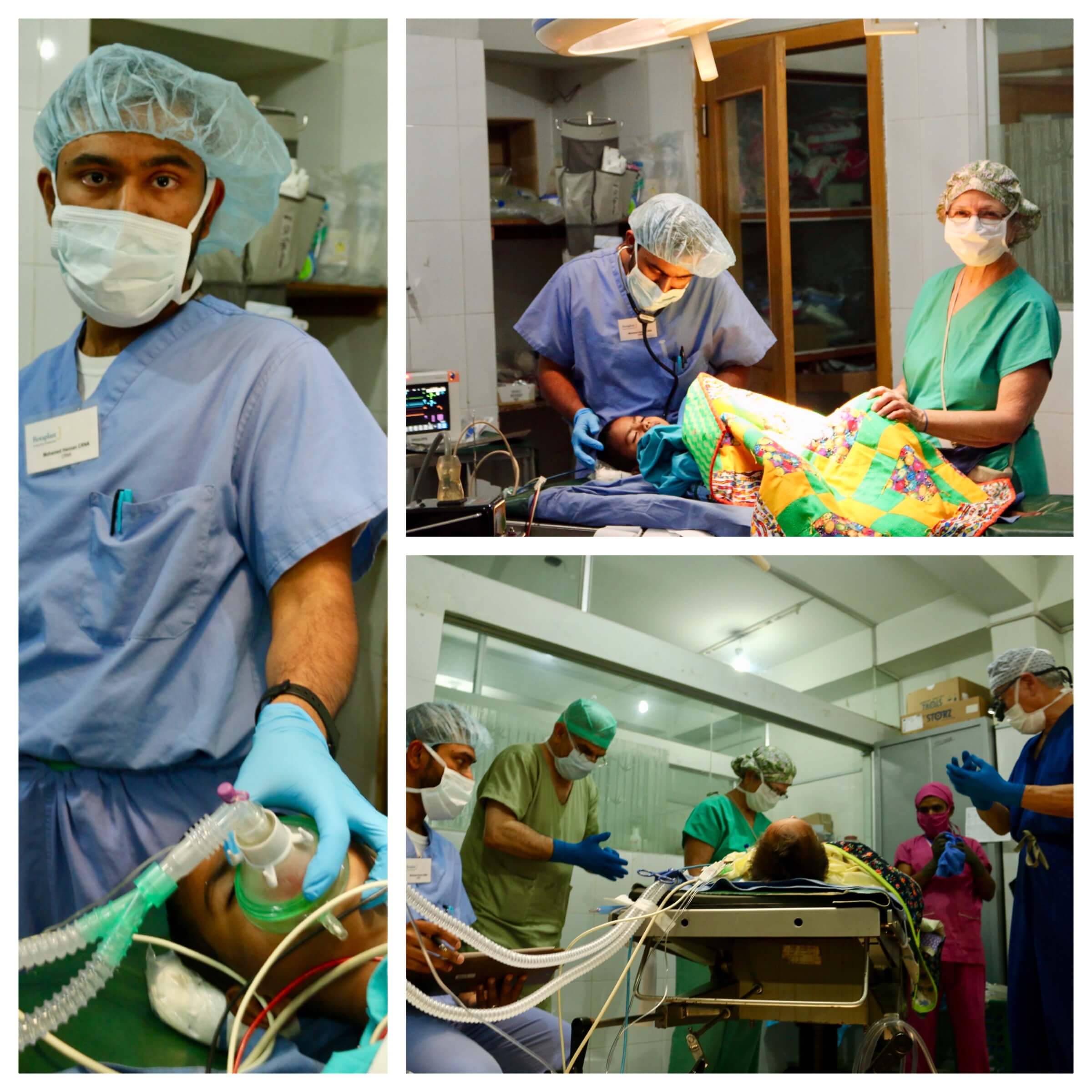
[Pictured: Mohammed Hannan with face mask, Mohammed Hannan and Marilyn Santiago monitoring patient, Mohamed Hannan, Adnan Uzunismail (Surgeon), Marilyn Santiago, local Scrub Nurse, and Wally Chang performing “time out”]
The patient will then be “intubated” which is to have a breathing tube so that an Anesthesiologist has direct access to ensuring the lungs continue to function and that the brain/body continue to get Oxygen throughout. The patient will be positioned, the area will be sterilized with Betadine, and drapes will cover the rest of the body so as to isolate the area for operation.
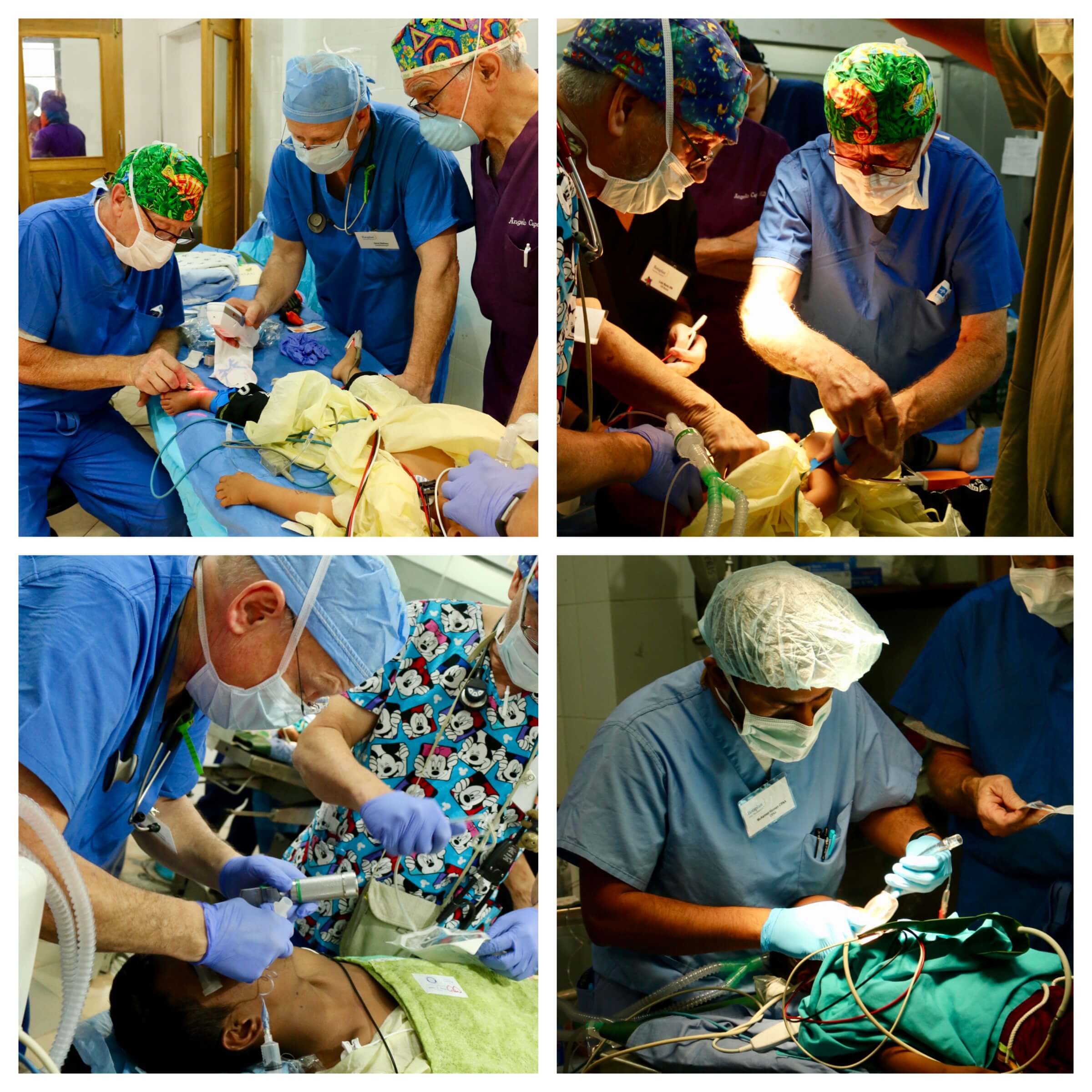
[Pictured: Joe Anderson (Lead Anesthesiologist), David Stellway, and Angelo Capozzi (Medical Director) search for a vein to start an IV. Michael Fallon and Joe Anderson starting an IV. Bottom: David Stellway and Mohammed Hannan intubating a patient]
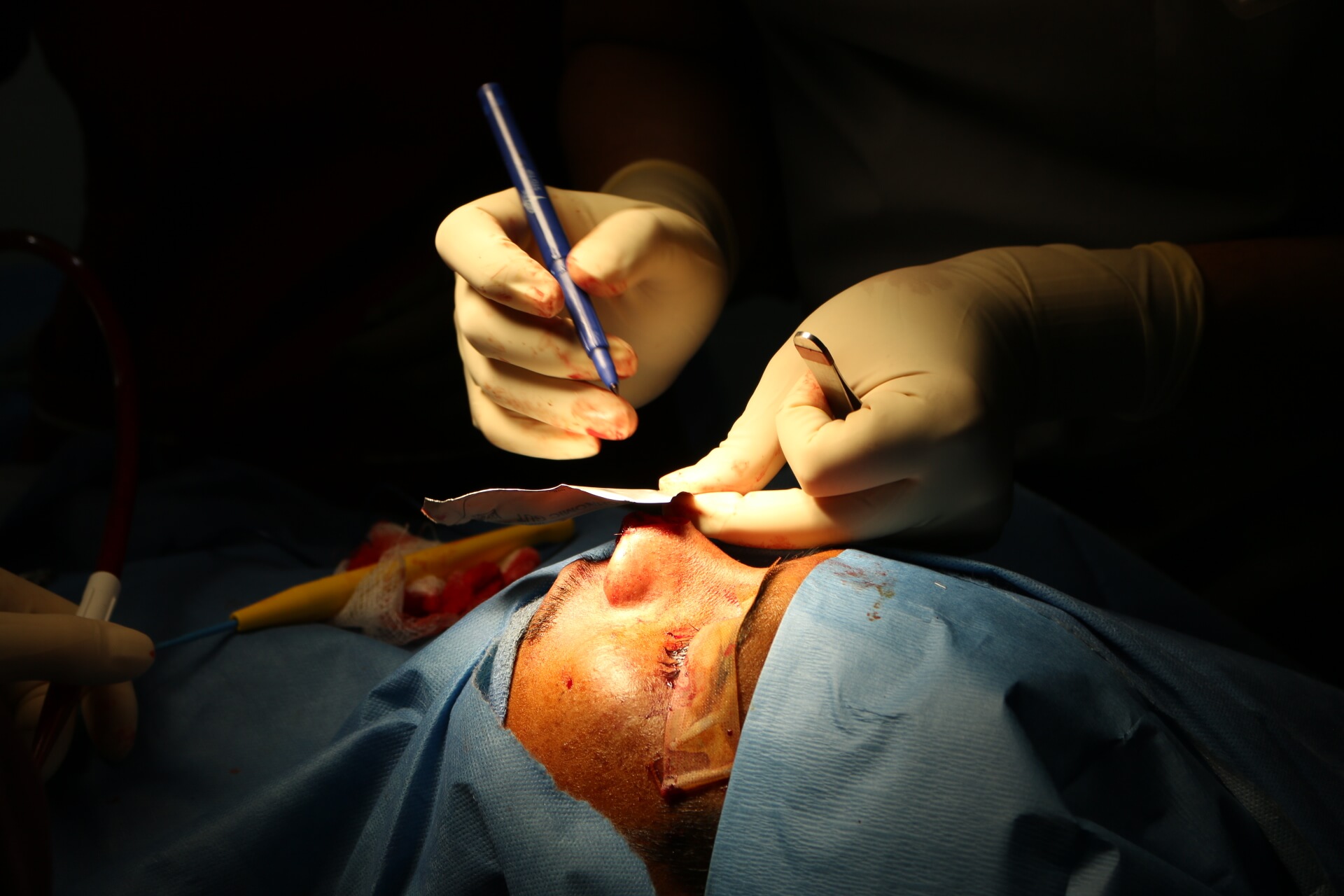
The Surgeon will “scrub in” fully sterilized and then proceed to start the operation using tools like a scalpel for cutting, a cauterizer for controlling blood loss, and needles/thread for sewing up the area. Sometimes more special tools are required. The Operating Room Nurses are critical for anticipating each piece of equipment the surgeon will need next to keep the procedure going.
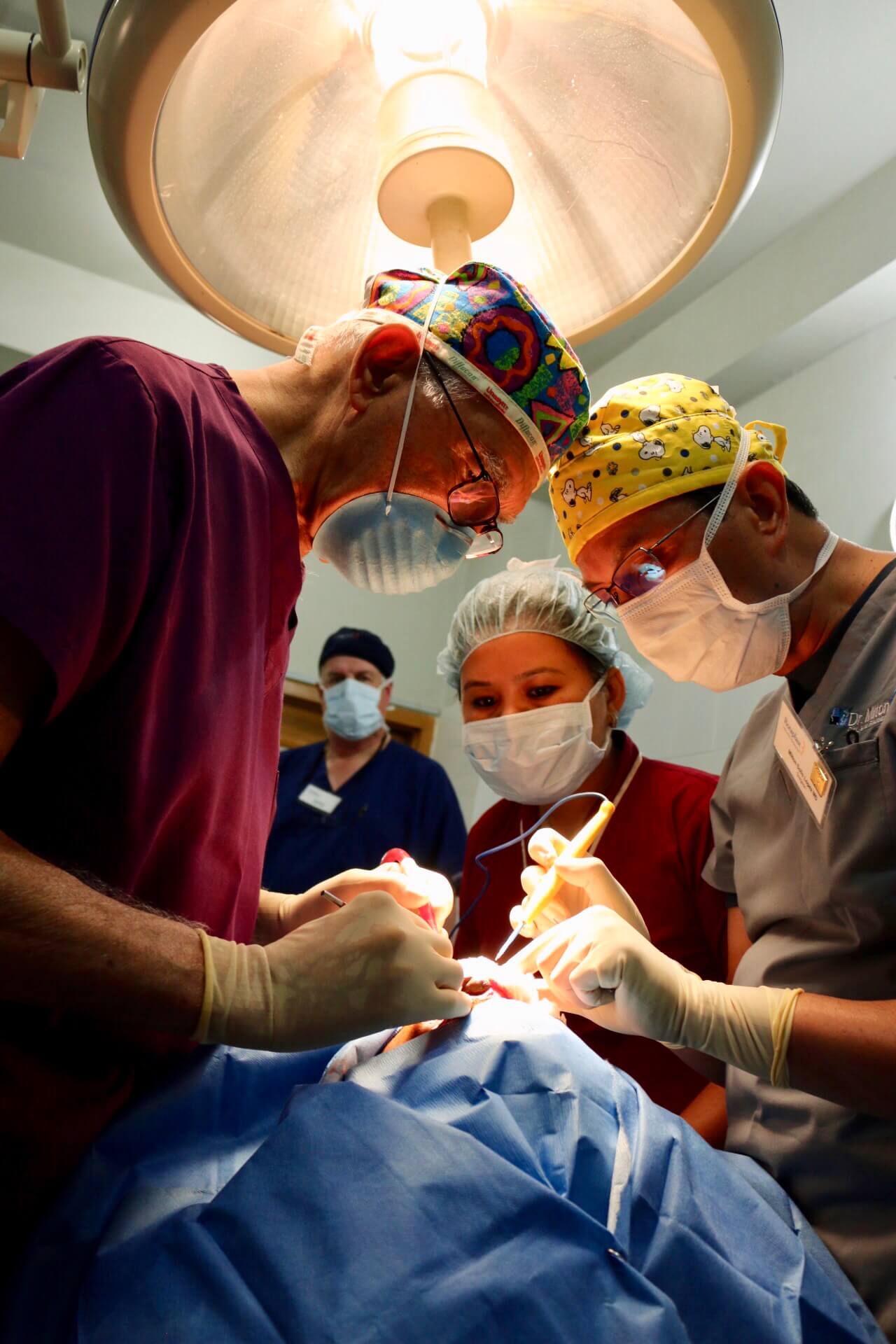
[Pictured: Angelo Capozzi, Randy Floyd, local scrub Nurse, Milton Solis]
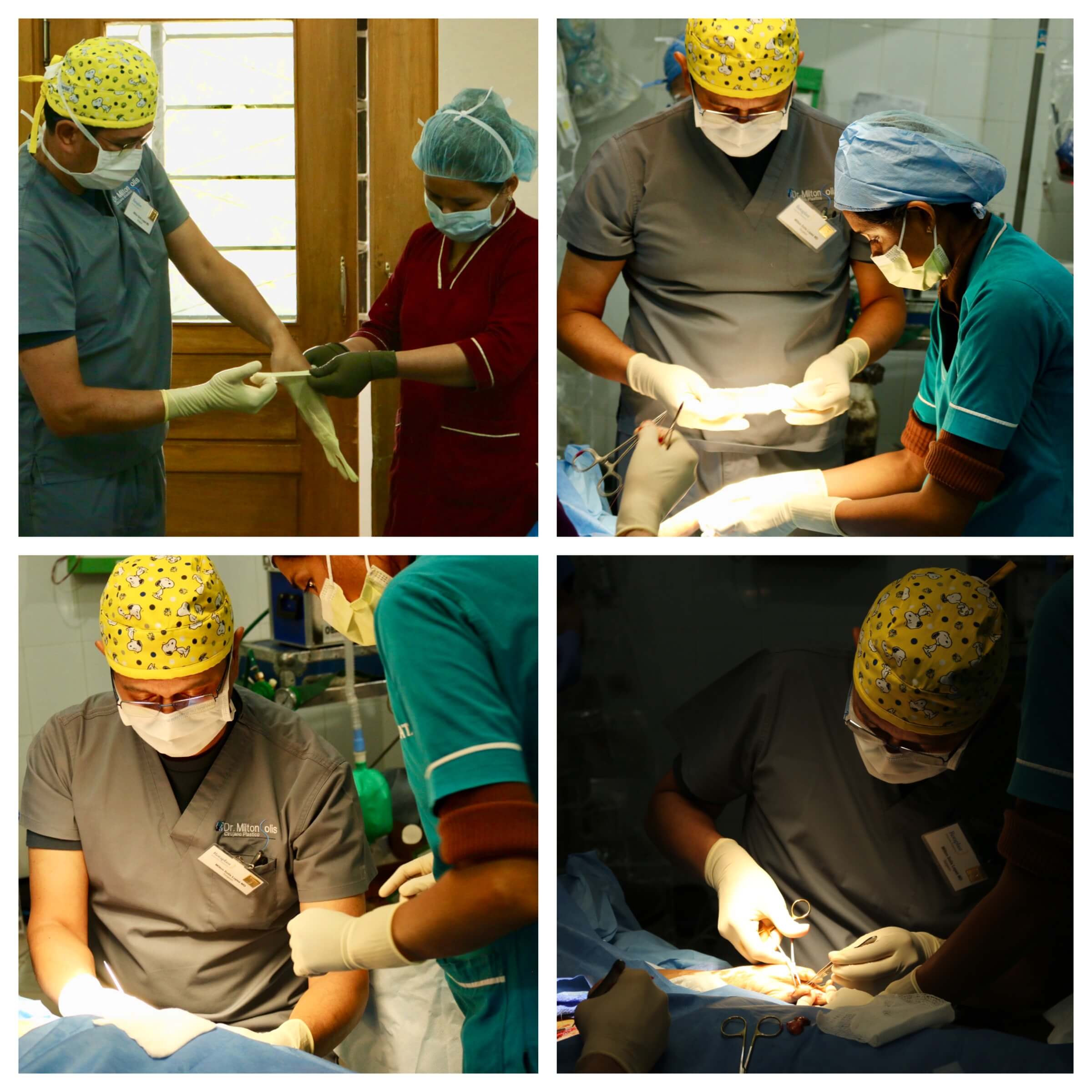
[Pictured: Milton Solis]
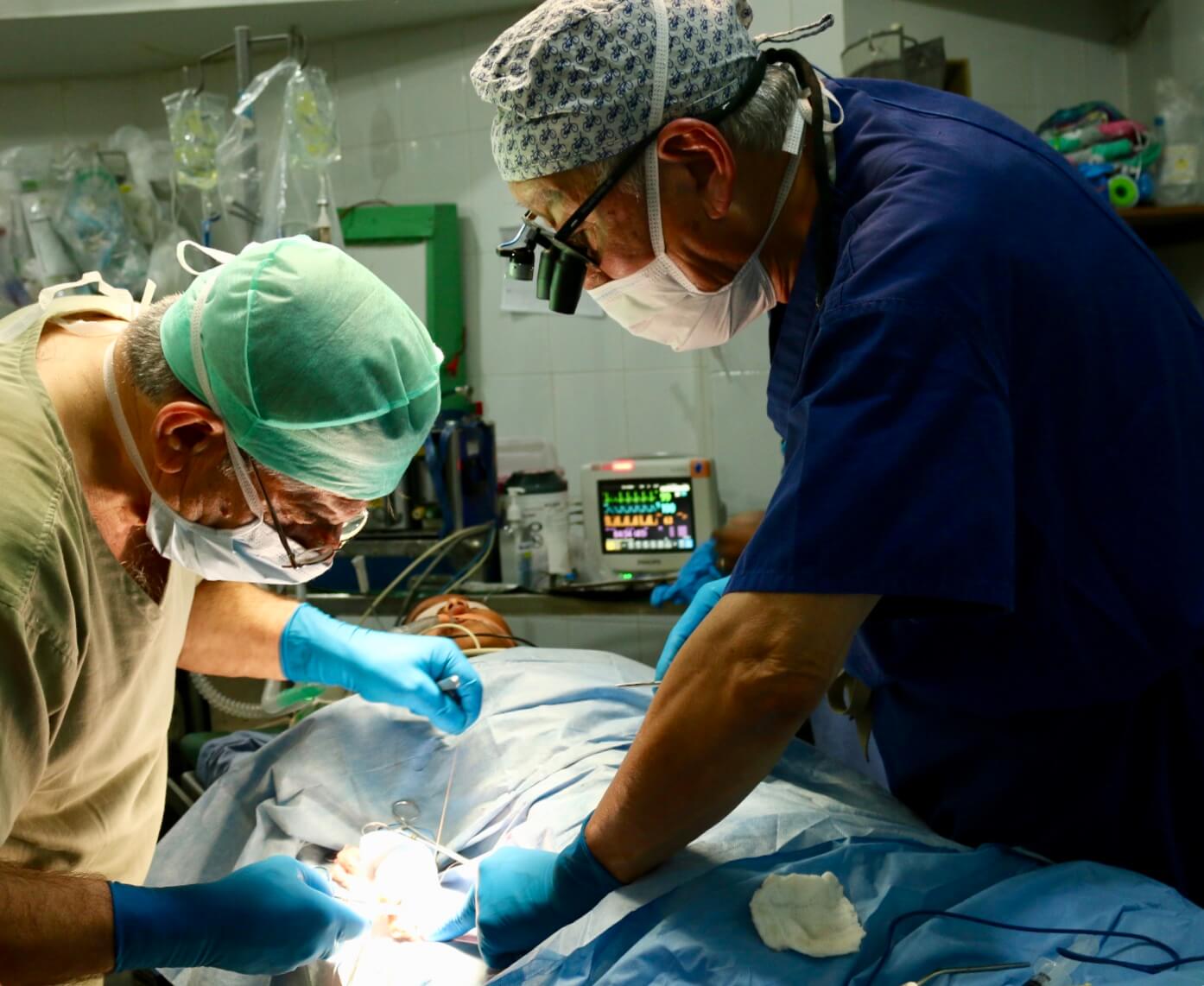
[Pictured: Adnan Uzunismail (green) and Wally Chang (blue)]
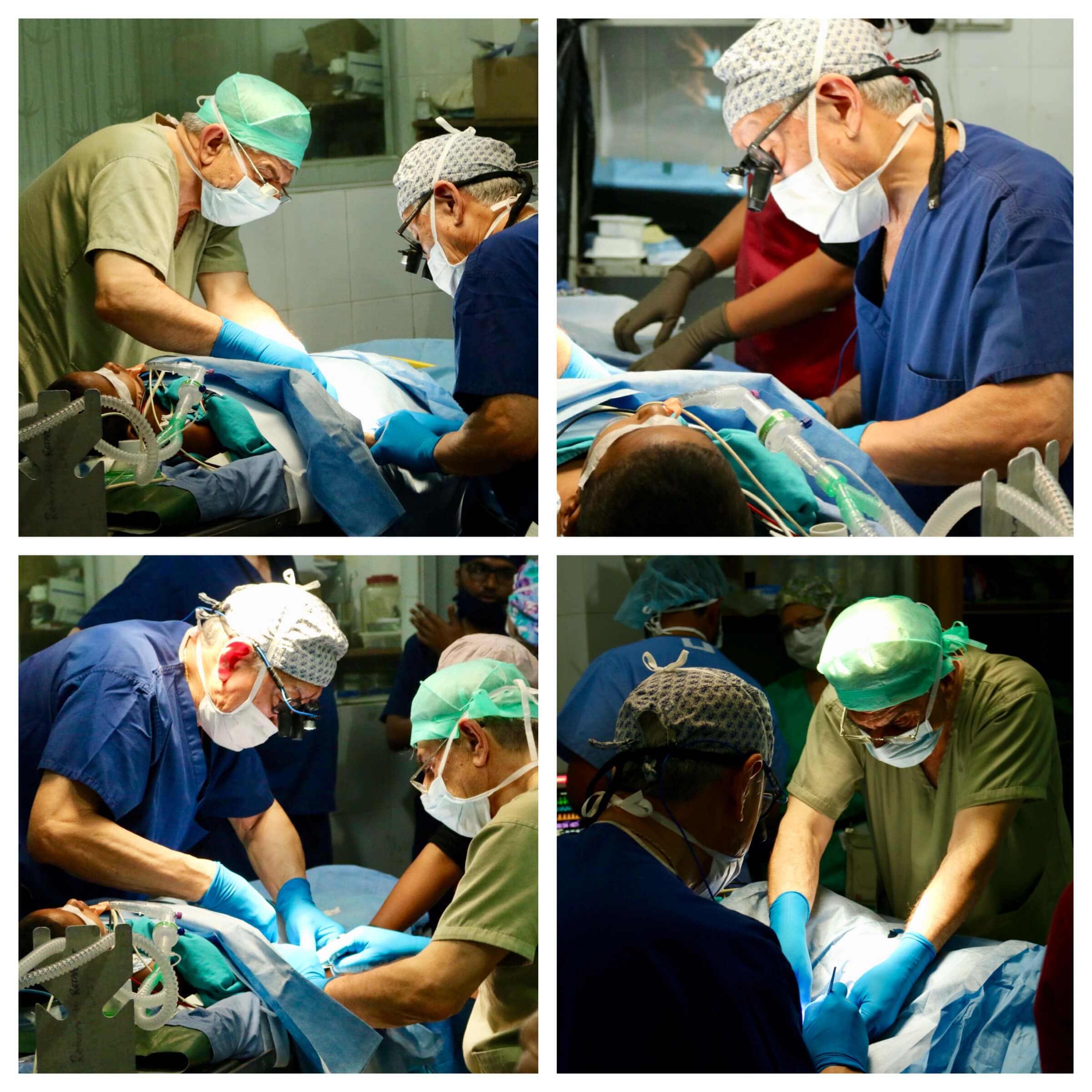
The entire time the Anesthesiologist watches the vitals, monitors trends, and intervenes with antibiotics and other anesthetics to control pain and nausea. They are charged with making sure the patient makes it through the operation safely. Once the operation is complete, dressings are administered, and anesthetic is decreased so that the patient can begin to awaken. The breathing tube is removed and the patient is taken to the Recovery room. The equipment is taken to be sterilized for a future surgery. The Head Nurse controls the schedule of inflow and outflow of patients.
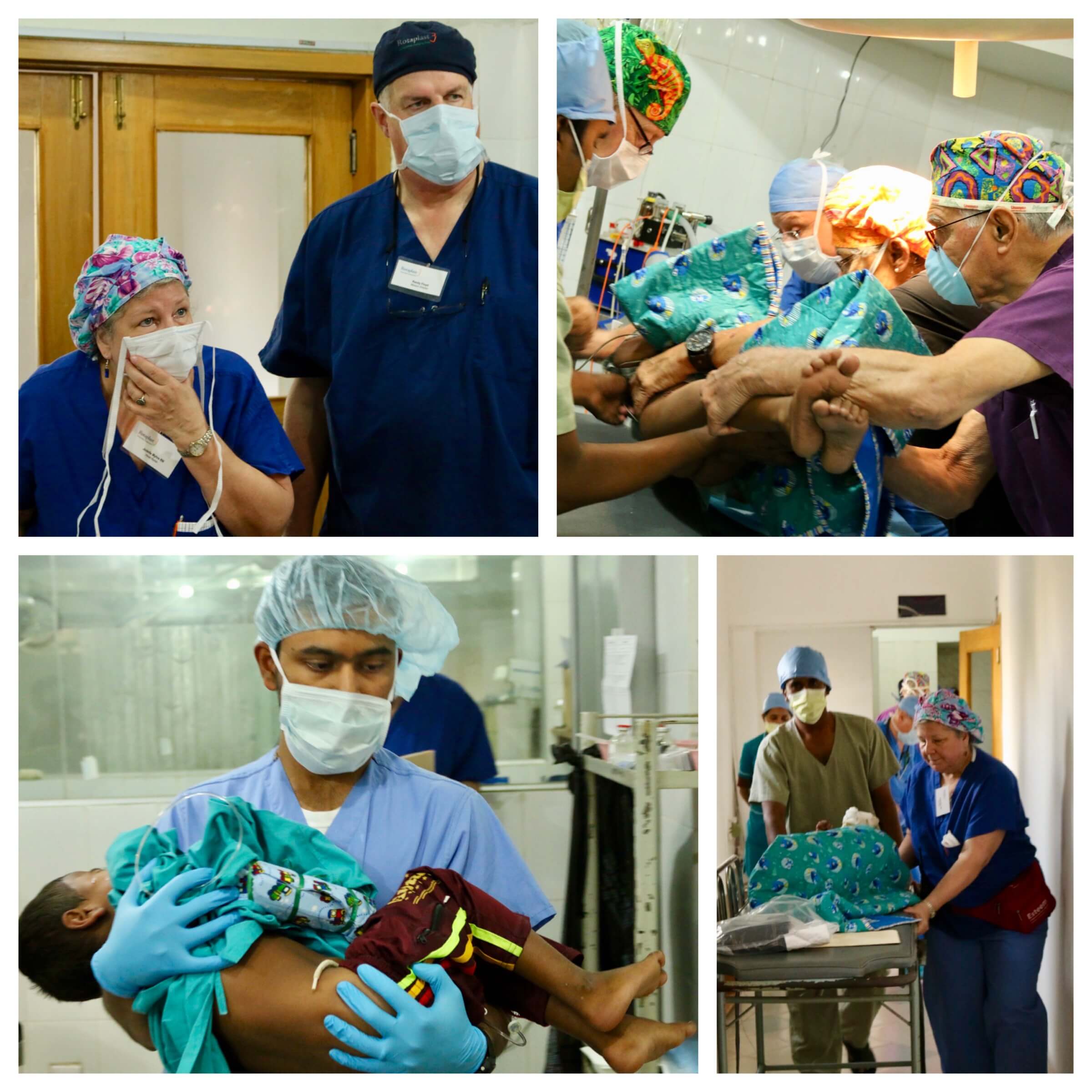
[Pictured: Jodelle Myhre (Head Nurse) and Randy Floyd. Transferring a patient: local Nurse, Joe Anderson, David Stellway, Lois Borie (OR Nurse), and Angelo Capozzi. Mohammed Hannan carrying patient out. Local nurse and Jodelle Myhre]
In Recovery, the patient is monitored for their transition into wakefulness. Vitals are taken and eventually if the patient is well enough to sit up and take fluids, the IV can be removed. The PACU Nurses soothe the patients to help their recovery. Shortly after they can be taken back to their supervised Ward where Nurses are on hand 24/7 to monitor their condition until the next day (depending on condition) where the Pediatricians and Surgeons come by to monitor progress and health before it is decided if they can be discharged.

[Picture T->B: Paula Fillari (Lead PACU Nurse) trying to soothe a patient with “Baby Shark”. Margaret Watson Hopkins (PACU Nurse) checking vitals. Paula Fillari adjusting a patient for comfort]